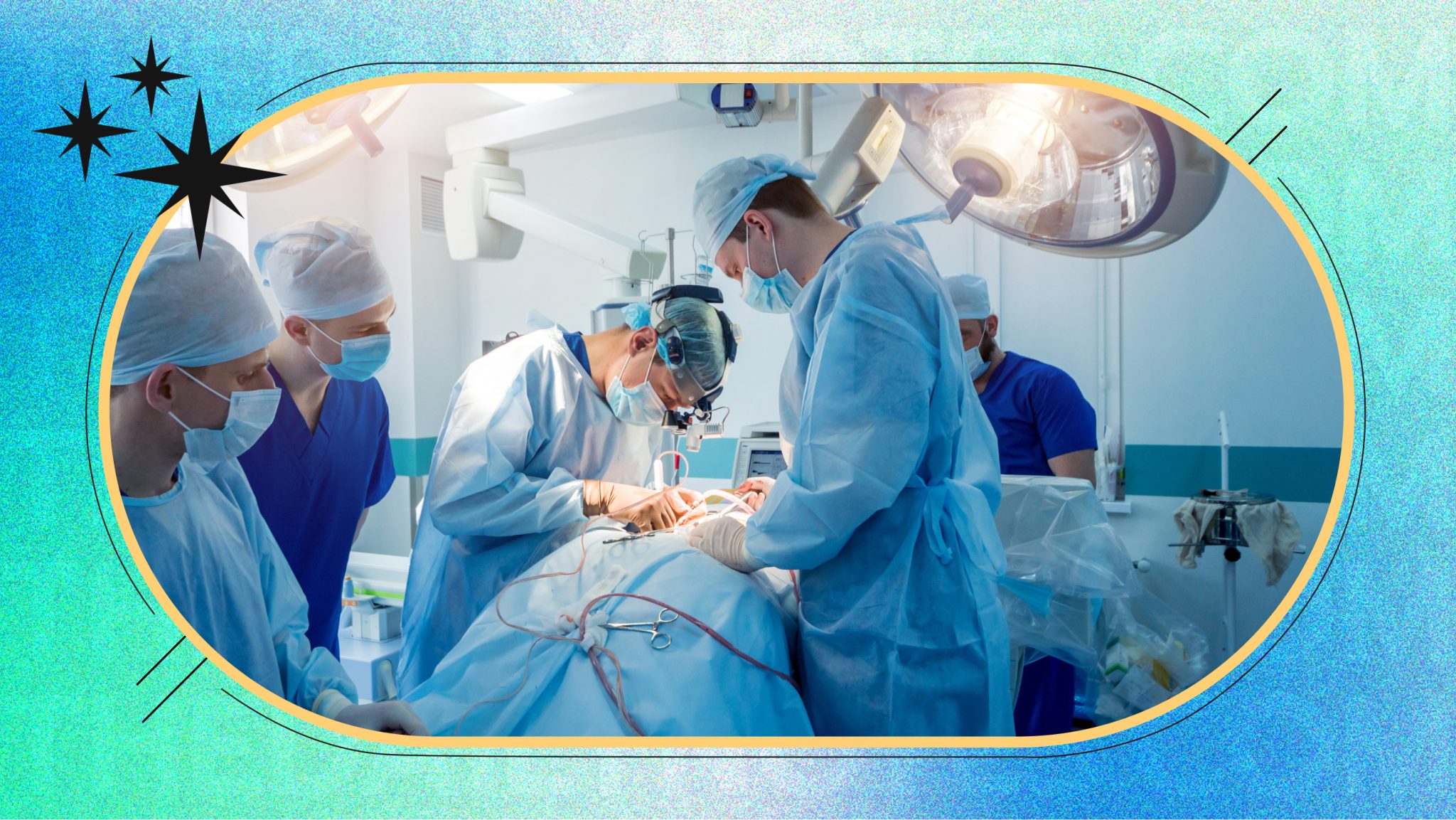
Kidney stones are a common and often painful condition affecting millions worldwide.
While some stones pass naturally, others require surgical intervention to prevent complications such as infection, kidney damage, or recurrent obstruction.
Understanding when kidney stone surgery is necessary is critical to protecting kidney function, reducing pain, and ensuring timely treatment.
This comprehensive guide explains kidney stones, symptoms, non-surgical management, indicators for surgery, types of surgical procedures, recovery expectations, risks, prevention, and long-term management strategies.
The information provided is designed to be accessible for patients while also informative for caregivers and healthcare professionals.
Understanding Kidney Stones
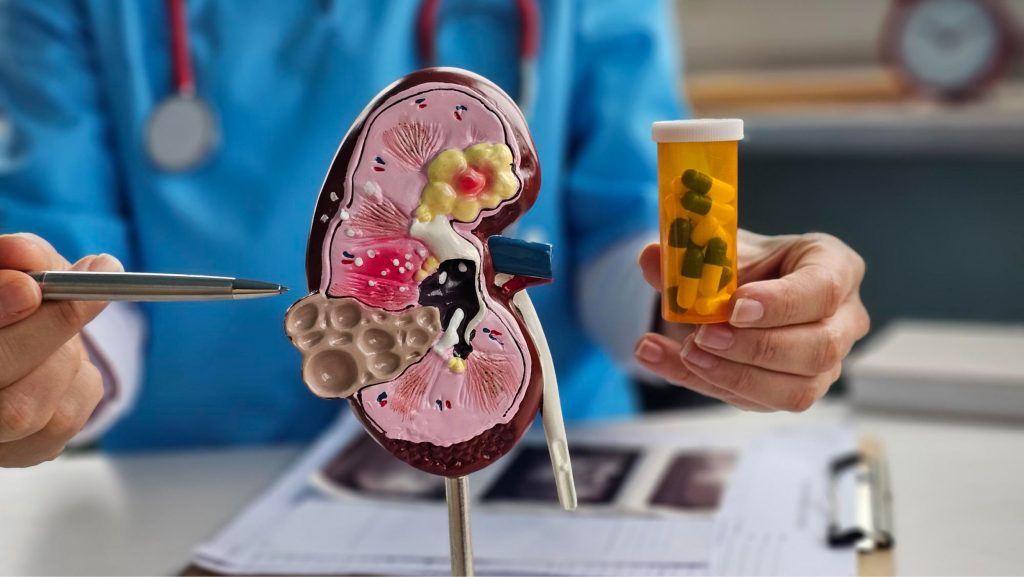
Kidney stones, or renal calculi, are solid masses made of crystals that form in the urinary tract. They develop when urine contains high concentrations of minerals such as calcium, oxalate, and uric acid, which crystallize and clump together. Over time, these stones can grow and cause blockage, pain, or kidney damage.
How Kidney Stones Form?
Stone formation is a multi-step process:
- Supersaturation of urine – Occurs when the concentration of stone-forming minerals exceeds the amount that can be dissolved.
- Crystal nucleation – Small mineral particles begin to stick together.
- Crystal growth – Crystals grow over time and may aggregate.
- Stone retention – Stones may remain in the kidney, grow, and eventually move into the ureter.
Several factors contribute to stone formation:
- Dehydration: Concentrated urine encourages crystallization.
- Diet: High intake of salt, sugar, animal protein, and oxalate-rich foods (e.g., spinach, nuts) increases risk.
- Genetics: Family history increases susceptibility.
- Medical conditions: Obesity, gout, metabolic syndrome, and urinary tract infections (for struvite stones) increase risk.
- Medications: Certain diuretics, antacids, or supplements may influence stone formation.
Types of Kidney Stones
The type of stone influences both treatment and prevention strategies.
- Calcium stones (most common)
- Usually calcium oxalate
- Linked to dehydration, high-oxalate diet, and metabolic factors
- Often form multiple small stones
- Uric acid stones
- Form in acidic urine
- More common in patients with gout or high-protein diets
- Can sometimes be dissolved with medication
- Struvite stones
- Caused by urinary tract infections
- Can grow rapidly and form large, branching stones (staghorn calculi)
- Require prompt removal to prevent kidney damage
- Cystine stones
- Rare, caused by a genetic disorder
- Form in patients with cystinuria
- Tend to recur throughout life
Symptoms of Kidney Stones
Symptoms vary depending on stone size, location, and movement.
Common Signs
- Sharp flank pain: Often described as excruciating, sometimes radiating to the lower abdomen or groin.
- Hematuria (blood in urine): Occurs when the stone irritates urinary tract lining.
- Painful urination: Especially when the stone moves into the ureter or bladder.
- Frequent urination or urgency: Irritation from a stone in the lower urinary tract.
- Nausea and vomiting: Caused by pain and the body’s stress response.
- Abdominal or groin discomfort: Can be intermittent, often worsening in waves (“renal colic”).
Red-Flag Symptoms Requiring Immediate Attention
- Fever and chills (possible infection)
- Inability to urinate
- Severe vomiting leading to dehydration
- Blood clots in urine
- Persistent, worsening pain unrelieved by medication
These indicate serious complications such as infection, obstruction, or kidney injury, and require urgent medical care.
Can Kidney Stones Pass Without Surgery?
Small stones often pass naturally without surgical intervention.
Stones Likely to Pass Naturally
- Stones less than 5 mm have up to a 90% chance of passing naturally.
- Stones 5–10 mm may pass with medication and hydration.
- Stones larger than 10 mm rarely pass and often require surgery.
Conservative Management Methods
- Hydration: Drinking 2–3 liters of water per day to flush stones.
- Pain management: NSAIDs or acetaminophen for discomfort.
- Alpha-blockers: Medications like tamsulosin relax ureter muscles to ease stone passage.
- Dietary modification: Reducing salt and oxalate intake depending on stone type.
- Monitoring: Imaging and urine tests to track stone movement.
Limitations of Non-Surgical Treatment
Conservative treatment may fail in cases of:
- Large stones (>10 mm)
- Severe obstruction
- Recurrent or persistent pain
- Infection
- Stones in problematic locations
If non-surgical approaches are ineffective, surgical intervention is recommended.
When Do You Need Surgery for Kidney Stones?
Surgery is indicated in several situations to protect kidney function, prevent infection, relieve pain, and improve quality of life.
1. Stone Size Is Too Large
Large stones are unlikely to pass on their own. Surgical removal is necessary for:
- Stones >6 mm, which rarely pass without assistance
- Stones >10 mm, almost always requiring intervention
Why it matters: Large stones can obstruct urine flow, lead to kidney swelling (hydronephrosis), and cause long-term damage.
2. Severe or Uncontrolled Pain
Persistent, severe pain despite medication suggests that the stone is lodged or obstructing urine flow.
Pain as an indicator:
- Pain interfering with daily life
- Pain unrelieved by NSAIDs or opioids
- Recurrent pain episodes
Surgical relief: Surgery immediately alleviates pain and reduces stress on the kidney.
3. Urinary Tract Obstruction
Obstruction occurs when the stone blocks the ureter, preventing urine from reaching the bladder.
Risks of untreated obstruction:
- Hydronephrosis (kidney swelling)
- Declining kidney function
- Increased risk of infection
Surgical intervention: Relieves obstruction and prevents permanent damage.
4. Recurrent or Severe Infections
Kidney stones can harbor bacteria, leading to recurrent UTIs.
Why infection necessitates surgery:
- Antibiotics alone are often insufficient
- Infection combined with obstruction can cause sepsis
- Surgical removal eliminates the source of infection
5. Kidney Function Is Declining
Persistent stones can reduce kidney efficiency.
Indicators for surgery:
- Worsening creatinine or eGFR in blood tests
- Imaging shows kidney swelling or scarring
- Chronic obstruction threatens kidney health
Early intervention prevents irreversible damage.
6. Failure of Non-Surgical Treatments
If conservative measures fail after several weeks:
- Stone remains in place
- Symptoms persist
- Hydration, medications, and lifestyle changes are ineffective
Surgery is recommended as the next step.
7. Stones in High-Risk Locations
Certain areas of the urinary tract make stone passage unlikely:
- Ureteropelvic junction
- Lower ureter
- Kidney calyces (small inner cavities)
Surgical removal prevents prolonged discomfort and complications.
Types of Kidney Stone Surgery
Surgery options have evolved significantly over the years, becoming minimally invasive, safe, and tailored to the size and location of the stone.
The choice of procedure depends on stone type, location, size, and patient health. Each type has unique benefits, limitations, and recovery considerations.
1. Extracorporeal Shock Wave Lithotripsy (ESWL)
Best for: Small to medium stones
How it works: ESWL uses focused shock waves from outside the body to break stones into smaller fragments, which can then pass naturally through the urinary tract.
The procedure is non-invasive and typically performed on an outpatient basis.
Advantages:
- Non-invasive, with no surgical incision
- Quick procedure time, often under one hour
- Minimal recovery time, allowing patients to resume normal activities quickly
Limitations:
- Less effective for stones larger than 2 cm or very hard stones
- May require multiple sessions if stones are resistant or if fragments remain
Patient tips:
- Hydration is crucial: Drinking plenty of fluids helps flush stone fragments
- Strain your urine: Collect fragments for analysis to guide future prevention
- Mild soreness may occur: Some flank discomfort or bruising is normal for a few days
Additional notes: ESWL may not be recommended for pregnant patients, those with severe obesity, or patients with bleeding disorders. It is most effective for stones located in the kidney or upper ureter.
2. Ureteroscopy (URS)
Best for: Stones in the ureter or kidney
Procedure: A thin, flexible ureteroscope is inserted through the urethra and bladder into the ureter or kidney.
A laser or small basket is used to fragment or remove the stone directly. This method is minimally invasive and avoids external incisions.
Advantages:
- High success rate with immediate stone removal
- No external incision, reducing infection and healing complications
- Can access stones in difficult locations, including mid and lower ureter
Limitations:
- A temporary stent is often placed to ensure urine flow and reduce swelling
- Mild post-operative discomfort, including urinary urgency and burning
Patient tips:
- Expect blood-tinged urine for a few days post-procedure
- Avoid heavy lifting or strenuous exercise while the stent is in place
- Follow your urologist’s instructions for stent removal, usually within 1–2 weeks
Additional notes: URS is especially useful for stones that cannot be treated effectively with ESWL.
Patients may experience some urinary frequency and mild discomfort, which typically resolves after stent removal.
3. Percutaneous Nephrolithotomy (PCNL)
Best for: Large or complex stones (>2 cm), staghorn calculi
Procedure: PCNL involves a small incision in the back, through which a scope is inserted directly into the kidney.
Stones are fragmented and removed in a single session, making it ideal for large or complex stones.
Advantages:
- Effective for large stones that are not suitable for ESWL or URS
- Often requires only one procedure to completely remove the stone
Limitations:
- Requires a hospital stay, usually 1–2 days
- Recovery is longer compared to ESWL or URS
- Small risk of bleeding or infection due to incision
Patient tips:
- Monitor for fever, severe pain, or excessive bleeding
- Follow up with imaging to ensure complete stone removal
- Maintain proper hydration and avoid strenuous activity during recovery
Additional notes: PCNL is particularly effective for staghorn stones that occupy a large portion of the kidney or multiple stones in different calyces.
While recovery is longer than other procedures, the success rate for complete stone clearance is very high.
4. Open or Laparoscopic Surgery
Rarely used today, reserved for:
- Complex stones in abnormal kidney anatomy
- Very large staghorn stones that cannot be accessed by minimally invasive methods
Recovery:
- Recovery is longer due to surgical incision or laparoscopic entry points
- Patients may need several weeks before returning to normal activity
Patient tips:
- Only considered when other less invasive methods are ineffective or impractical
- Pain management and wound care are critical in the first 1–2 weeks
- Close follow-up is required to monitor kidney function and healing
Additional notes: Open or laparoscopic surgery is now uncommon thanks to ESWL, URS, and PCNL.
However, it remains necessary in rare cases, such as congenital kidney anomalies or unusually large stones resistant to other treatments.
Recovery After Kidney Stone Surgery
Recovery after kidney stone surgery varies significantly depending on the type of procedure, size and location of the stone, and the overall health of the patient.
Understanding what to expect can help patients plan for a smoother recovery, reduce complications, and return to normal activities safely.
Short-Term Recovery
Short-term recovery refers to the period immediately following surgery, typically the first few hours to a few days.
Common experiences during short-term recovery include:
- Mild flank or abdominal pain:
- Pain is most noticeable at the surgical site or where the stone was located.
- ESWL may cause soreness as fragments move through the urinary tract.
- URS or PCNL may result in localized pain from the procedure or stent placement.
- Pain can usually be managed with prescribed or over-the-counter pain medication.
- Blood in urine (hematuria):
- Slightly pink or reddish urine is common in the first few days post-surgery.
- Blood should gradually decrease over time. If bleeding becomes heavy or persistent, patients should contact their doctor immediately.
- Discomfort during urination:
- A burning sensation or mild urgency can occur, especially if a stent was placed.
- Drinking plenty of water helps flush the urinary tract and reduce irritation.
- Swelling or bruising at incision sites (for PCNL or open surgery):
- Patients may notice minor swelling, redness, or tenderness at the back or flank area.
- Applying ice packs (if recommended) and avoiding strenuous activity helps reduce swelling.
- Fatigue or low energy:
- Patients may feel tired due to anesthesia and the body’s healing process.
- Short naps, rest, and gradual resumption of activities are encouraged.
Long-Term Recovery
Long-term recovery focuses on the weeks following surgery, including monitoring complications and ensuring full kidney and urinary function.
Key aspects include:
- Follow-up imaging:
- Doctors typically schedule ultrasound, X-ray, or CT scans to confirm complete stone removal and check for residual fragments.
- Imaging may occur 1–4 weeks after surgery depending on the procedure.
- Normalization of pain and urinary function:
- Mild discomfort should gradually resolve.
- Urination should return to normal without burning or urgency.
- Any persistent symptoms such as fever, severe pain, or blood in urine require prompt medical attention.
- Return to normal activities:
- ESWL: Most patients can resume daily activities within 1–2 days. Light exercise is generally safe.
- URS: Recovery may take 2–4 days. Patients with stents may have mild urinary discomfort during this period.
- PCNL: Recovery can take 1–2 weeks due to the incision. Heavy lifting and strenuous activity should be avoided until cleared by a doctor.
- Open or laparoscopic surgery: Recovery may take 2–4 weeks depending on the complexity of the procedure.
Tips for a Smooth Recovery
1. Stay hydrated:
- Drinking plenty of water helps flush remaining stone fragments and prevents new stone formation.
2. Pain management:
- Take prescribed painkillers as directed. Avoid excessive use of NSAIDs if recommended by your doctor.
3. Monitor urine:
- Watch for blood, clots, or unusual color. Straining urine to catch fragments may be recommended.
4. Avoid heavy lifting or strenuous exercise:
- Sudden strain may disrupt healing, especially after PCNL or open surgery.
5. Follow dietary recommendations:
- Continue preventive measures such as reduced salt, moderate protein, and sufficient fluids.
6. Take care of incisions and stents:
- Keep the surgical area clean and dry. Follow instructions for stent care and removal.
7. Report complications immediately:
- Fever, persistent pain, severe bleeding, inability to urinate, or infection signs should be addressed promptly.
Expected Recovery Timelines by Procedure
| Procedure | Recovery Time | Notes |
|---|---|---|
| ESWL | 1–2 days | Mild soreness, blood in urine as fragments pass |
| URS | 2–4 days | Stent may cause temporary discomfort |
| PCNL | 1–2 weeks | Small incision, possible swelling and bruising |
| Open Surgery | 2–4 weeks | Only for complex cases; longer healing needed |
Return to Work and Daily Life
- Most patients undergoing ESWL or URS can return to work and light daily activities within a few days.
- For PCNL or open surgery, return to work may take 1–2 weeks depending on activity level.
- Avoid high-impact sports, heavy lifting, or activities that strain the back or abdomen until fully cleared by a doctor.
Long-Term Follow-Up
Recovery does not end after pain resolves. Long-term follow-up is essential for:
- Monitoring kidney function with blood tests
- Detecting new stones early through imaging or urine tests
- Ensuring lifestyle changes are effective in preventing recurrence
- Adjusting medications if stone risk persists
Patients with a history of recurrent stones or metabolic conditions may require annual evaluations.
Preventing Future Kidney Stones
While kidney stone surgery effectively removes existing stones, it does not prevent new stones from forming.
Recurrence is common, with studies showing that up to 50% of patients may develop another stone within five years if preventive measures are not followed.
Fortunately, a combination of lifestyle changes, dietary modifications, and medical management can dramatically reduce the risk of future stones.
1. Lifestyle and Dietary Strategies
Lifestyle and diet play the most significant role in preventing kidney stones. Small daily adjustments can have a big impact on urinary health.
Hydration: Drink Plenty of Water
- Aim for 2–3 liters (8–12 cups) of water per day, unless otherwise directed by your doctor.
- Adequate hydration dilutes urine, preventing minerals from crystallizing and forming stones.
- Monitor urine color: pale yellow urine indicates proper hydration, while dark yellow or amber suggests you need more fluids.
- Tips to increase water intake:
- Carry a water bottle throughout the day
- Drink a glass of water with every meal
- Add natural flavorings like lemon slices to encourage more water consumption
Note: People with heart or kidney conditions should consult a doctor before increasing fluid intake significantly.
Limit Salt (Sodium) Intake
- Excess sodium increases calcium levels in urine, which can contribute to calcium-based stones.
- Avoid processed foods, canned soups, salty snacks, and restaurant meals high in salt.
- Use herbs, spices, and citrus to flavor food instead of salt.
Tip: Check nutrition labels aim for less than 2,300 mg of sodium per day or as advised by your physician.
Moderate Animal Protein Intake
- High consumption of red meat, poultry, and seafood increases uric acid levels and acidity in urine, raising the risk of uric acid stones.
- Recommendations:
- Limit animal protein to one serving per meal
- Include plant-based protein sources such as beans, lentils, and tofu
Tip: Balance meals with fruits and vegetables to reduce urinary acidity.
Control Oxalate Intake (for Calcium Oxalate Stones)
- Oxalate binds with calcium in urine to form stones. Common high-oxalate foods include spinach, rhubarb, beetroot, nuts, chocolate, and tea.
- Moderate oxalate intake rather than eliminating it completely. Pairing oxalate-rich foods with calcium-rich foods helps prevent stone formation.
Example: Eat spinach with low-fat cheese or yogurt to bind oxalate in the gut.
Maintain a Healthy Weight and Exercise Regularly
- Obesity and sedentary lifestyle are linked to higher kidney stone risk.
- Aim for at least 150 minutes of moderate-intensity exercise per week (e.g., walking, swimming, cycling).
- Maintain a healthy body weight and BMI, as metabolic syndrome increases the risk of uric acid stones.
Tip: Even short walks after meals improve digestion and overall kidney health.
Limit Sugar and Processed Foods
- High sugar intake, particularly fructose and sugary drinks, increases uric acid and stone risk.
- Reduce consumption of soft drinks, energy drinks, and sugary desserts.
- Opt for whole fruits instead of juices, which contain concentrated sugars.
Include Citrate-Rich Foods
- Citrate helps prevent stone formation by binding calcium in urine.
- Foods high in citrate include lemons, limes, oranges, and grapefruit.
- Adding lemon or lime juice to water daily can be a simple preventive measure.
2. Medical Prevention
For patients at high risk or those with recurrent stones, medical management is often recommended.
Medications May Adjust Urine Chemistry
- Potassium citrate: Increases urinary citrate, reducing calcium stone formation.
- Thiazide diuretics: Reduce calcium excretion in urine.
- Allopurinol: Lowers uric acid levels in patients prone to uric acid stones.
Tip: Always take medications as prescribed and have urine and blood tests periodically to monitor effectiveness.
Regular Check-Ups and Urine Testing
- Follow-up visits help monitor for new stone formation and evaluate kidney function.
- 24-hour urine collection can analyze mineral content and pH, helping doctors customize preventive strategies.
- Imaging (ultrasound, CT scan) may be recommended for high-risk patients to detect stones early.
Stone Analysis After Surgery
- Analyzing the composition of removed stones provides critical information for prevention.
- Different stone types require different dietary and medical strategies:
- Calcium oxalate stones: reduce oxalate, moderate calcium
- Uric acid stones: reduce protein, alkalize urine
- Struvite stones: prevent infections
- Cystine stones: increase fluids and use cystine-binding drugs
3. Lifestyle Habits Beyond Diet
Other small daily habits can support kidney health:
- Avoid prolonged dehydration: Especially during exercise or hot weather.
- Limit excessive vitamin C supplements: Large doses can increase oxalate production.
- Monitor over-the-counter medications: Some antacids and supplements can affect urine chemistry.
- Do not ignore symptoms: Early treatment of pain, hematuria, or urinary discomfort prevents complications.
4. Long-Term Follow-Up and Monitoring
- Patients with a history of kidney stones should maintain regular follow-ups with a urologist or nephrologist.
- Urine testing, blood work, and imaging help detect early recurrence.
- Long-term monitoring is especially important for patients with metabolic disorders, recurrent stones, or complex stone types.
When to Seek Immediate Medical Care?
Seek urgent attention if:
- Fever with stone pain (possible infection)
- Inability to urinate
- Severe vomiting
- Signs of sepsis or kidney failure
Delaying treatment can cause life-threatening complications.
FAQs
Here are a few questions and queries on the topic of surgery for kidney stones that others have asked, and you might think helpful at the same time.
1. Can kidney stones go away without surgery?
Yes, many kidney stones, especially those smaller than 5 mm, often pass naturally through the urinary tract.
Drinking plenty of water, taking pain-relieving medications, and using prescribed alpha-blockers to relax the ureter can help the stone pass.
However, stones larger than 6 mm rarely pass on their own and may require surgical intervention to prevent complications.
2. How painful is kidney stone surgery?
Modern kidney stone surgeries are generally minimally invasive, and patients receive anesthesia to prevent pain during the procedure.
Post-operative discomfort is usually mild and manageable with over-the-counter pain medication or prescription analgesics.
ESWL may cause temporary flank pain as fragments pass, while URS or PCNL might involve mild soreness at the incision or stent site.
3. Is kidney stone surgery risky?
When performed by experienced urologists, the risks are low. Potential complications may include:
- Minor bleeding
- Temporary urinary discomfort
- Infection
- Rare injury to the urinary tract
Pre-operative tests and careful monitoring significantly reduce these risks. Your doctor will discuss the procedure-specific risks before surgery.
4. How long does surgery take?
The duration depends on the type of procedure and the size/location of the stone:
- ESWL: 30–60 minutes
- Ureteroscopy (URS): 1–2 hours
- Percutaneous Nephrolithotomy (PCNL): 1–3 hours
Recovery time varies, with ESWL allowing a return to normal activities within 1–2 days, URS in 2–4 days, and PCNL in 1–2 weeks.
5. Can stones recur after surgery?
Yes, kidney stones can recur if preventive measures are not followed. Recurrence depends on diet, hydration, genetics, and underlying health conditions.
Preventive strategies include drinking sufficient water, limiting salt and protein intake, and following doctor-recommended dietary or medical adjustments based on stone type.
6. How do I prepare for kidney stone surgery?
Preparation varies with the procedure:
- Fasting: Usually required 6–8 hours before surgery
- Medication adjustments: Blood thinners may need to be paused
- Pre-operative tests: Blood work, urine tests, and imaging
- Hydration: Some procedures may require limiting fluids temporarily
Your surgeon will provide detailed instructions for a safe and successful procedure.
7. What can I expect after surgery?
After surgery, patients may experience:
- Mild pain or soreness at the incision or stent site
- Blood-tinged urine for several days
- Temporary difficulty urinating or urinary urgency
- Fatigue, which generally improves within a few days
Your doctor may recommend hydration, rest, and follow-up imaging to ensure complete stone removal.
8. Will I need a stent after surgery?
A ureteral stent is sometimes placed temporarily after URS or PCNL to:
- Promote urine flow
- Reduce swelling in the ureter
- Facilitate healing
Stents are usually removed within a few days to weeks, depending on your procedure and recovery progress.
9. Can I prevent future kidney stones?
Yes, prevention is possible. Key strategies include:
- Drinking 2–3 liters of water daily
- Reducing salt and excessive animal protein
- Avoiding high-oxalate foods (for calcium oxalate stones)
- Maintaining a healthy weight
- Taking medications prescribed to reduce recurrence risk (e.g., potassium citrate for uric acid stones)
Regular follow-ups with your doctor and urine testing help track your risk.
10. Are there alternatives to surgery if stones are too large to pass naturally?
Yes, besides surgery, some options may be considered depending on stone size, location, and composition:
- Medical expulsive therapy: Using medications to relax ureter muscles
- Shock wave therapy (ESWL): Breaks stones into smaller fragments
- Combination approaches: Sometimes ESWL is combined with URS or stent placement
Your doctor will choose the safest and most effective option based on your specific situation.
11. How soon will I feel relief from pain after surgery?
Pain relief depends on the procedure:
- ESWL: Relief may occur gradually as stone fragments pass
- URS or PCNL: Pain relief is often immediate after stone removal
- Pain during urination or mild flank soreness may persist for a few days, but it generally improves with time and hydration.
12. Can kidney stones affect my kidney function permanently?
If left untreated, large or obstructive stones can damage kidney tissue over time, leading to reduced function or chronic kidney disease.
Timely surgical intervention prevents long-term damage and preserves kidney health. Regular monitoring post-surgery ensures kidney function remains optimal.
13. When should I contact my doctor after surgery?
Contact your doctor immediately if you experience:
- High fever or chills
- Severe or worsening pain
- Inability to urinate
- Heavy bleeding in urine
- Signs of infection at incision sites
Prompt attention prevents complications and ensures smooth recovery.
Surgery For Kidney Stones
Surgery becomes necessary for kidney stones when they are large, obstructive, infected, or causing kidney damage.
Modern minimally invasive techniques make treatment safe and effective, allowing rapid recovery and relief.
Patients can prevent recurrence through hydration, diet, medication, and regular follow-up.
Understanding when kidney stone surgery is required empowers patients to make informed decisions, seek timely care, and protect long-term kidney health.